We will discuss the following aspects. Please scroll down and start reading (and enjoy !):
- What are capacitors and why we use them in defibrillators.
- How capacitors are charged and discharged.
- How the defibrillator creates the “biphasic truncated exponential waveform”.
- A brief introduction to “automated external defibrillator” (AED).
- A brief introduction to “implantable cardioverter defibrillator” (ICD).
Introduction
We all know that electrical currents can kill a person. However, electrical current given using defibrillators can save lives. The human heart can develop an extremely serious condition called “ventricular fibrillation”, which if not treated, leads to death in minutes. A defibrillator is a device which, as its name suggests, can stop ventricular fibrillation. If you are not a medical person and want to know simply, what ventricular fibrillation is and how defibrillation stops it, please click here.
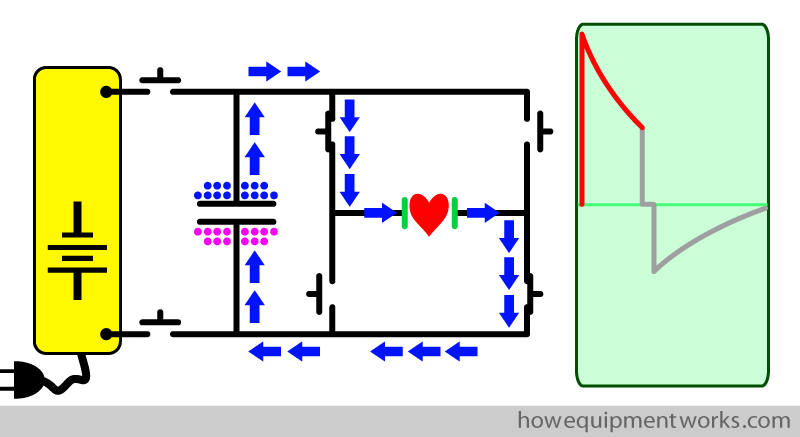
On this page of the website, you will learn the basic physics of how a defibrillator works. In the end, you will be able to understand and draw the basic circuit of a defibrillator as shown below. Please do not get a heart attack seeing this diagram! I will explain it step by step and you will understand it all.

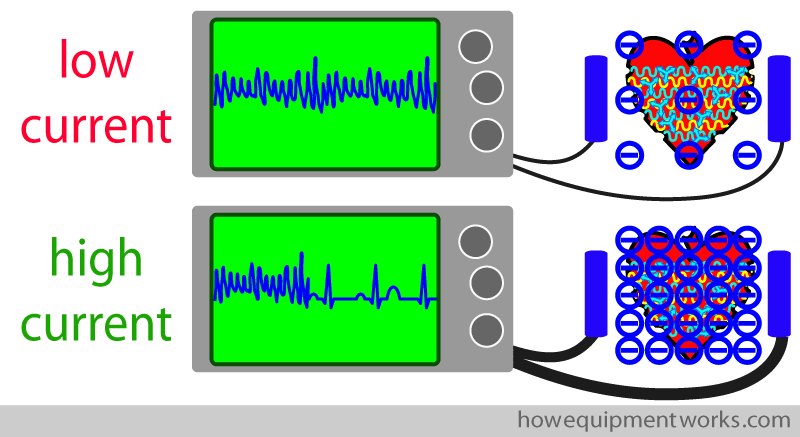
To defibrillate a heart, one needs to pass a very large current through the heart to silence the heart muscle cells. A low current would not work.
The need for a “capacitor”
A major design requirement of defibrillators therefore is to have the ability to provide the large current needed to defibrillate a heart. A crucial electrical component in defibrillators that makes it possible to deliver huge currents is a device called a “capacitor”.
To explain what a capacitor is, I would like you to imagine that you are a fireman (or firewoman!). Shown below is you, proudly wearing your red fireman’s uniform. Next to you is a water pipe, which of course will be your main weapon to combat any fires you will face. Like all visitors to this website, you are a dedicated worker and are happily waiting for your first fire.

While waiting for the first fire to happen, you decide to test your equipment. You turn on the water supply and to your surprise, the water flow is very low. Thinking that there must be some fault, you immediately tell your boss about it. She tells you that, to save money, she will only provide a low flow of water. You plead with her for a higher water flow, and all she says in response is; “No !”

While you were arguing with your boss, a real fire needs your urgent attention. You run with the water pipe and let the water flow into the fire.

Well, you are not surprised that the low water flow is not putting the fire out. Just as you told your boss, the water flow is simply not enough to put the fire out. In fact it appears that the fire is laughing at you!

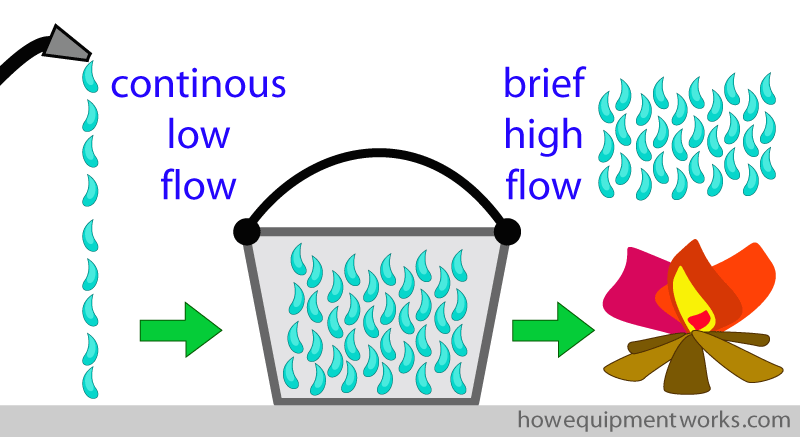
You are not the type who gives up and you start to think about a solution. The water that is being supplied to you is coming at a continuous low flow. However, what you need is a brief high flow of water that will once and for all put the fire out.

You suddenly think of a great solution. With your own money (you know your boss won’t give you any) you buy a bucket! You then do the following things. I will show the things you do in some detail as it will be relevant when we discuss the role of the capacitor in defibrillators. First, using the “continuous low flow” supply of water, you start filling the bucket.

After a little while, you have a bucket that has been filled with enough water to put the fire out.

Now you tip the bucket over the fire. A brief but high flow of water falls onto the fire, putting it out. You have won the battle! Your boss is happy and “promises” to pay for the bucket someday.

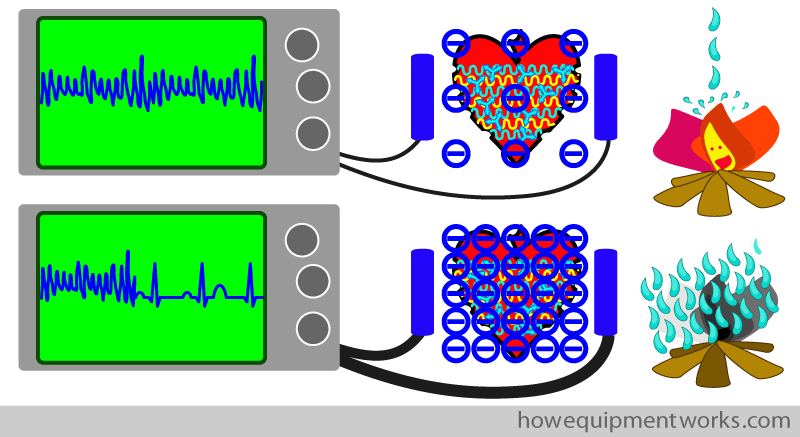
Now that you have put the fire out, let us return to defibrillators. As you may have guessed, there are some “similarities” between putting the fire out and defibrillation. As a fireman, to successfully put the fire out, you needed a brief large flow of water. In a similar way, as you learnt earlier in our discussion, you need a brief large current to defibrillate a heart.
You will recall that when you were a fireman, the big problem you had was that the water supply provided to you had a very low flow. Without the bucket, this low water flow was simply not enough to put the fire out. The bucket was your saviour!
The designers of defibrillators face a similar problem to the low-flow water supply you faced as a fireman. All electronic devices, including defibrillators, need a source of power (current) to work. For example, because defibrillators have to be easy to transport, they often get their power from batteries. Unfortunately, batteries can only produce a continuous low flow of current. The defibrillator has to “somehow” use the continuous low-flow current from the batteries to provide the brief high-flow current needed for defibrillation.

Defibrillators can also get power from the wall sockets in your hospital. However, even the maximum current available from such wall plugs is not enough to directly produce the high current flow required for defibrillation. I will further explain this.

As a very approximate example, the current needed for defibrillation can be in the region of 20 A (Amperes). So how big is a current of 20 A? Shown below is a diagram of a table lamp. A modern lamp such as this consumes about 0.02 Amperes.

As shown below, when you do the calculations, you will see that the 20 A defibrillation current equals the current consumed by approximately 1000 table lamps! So even when the defibrillator is plugged into a wall power socket, the current from the socket cannot be used directly to provide the huge current needed for defibrillation. How the defibrillator is able to produce the large currents needed for defibrillation from batteries or wall power sockets involves some magic which I will reveal to you soon! By the way, please do not learn the numbers shown below as they are very approximate.

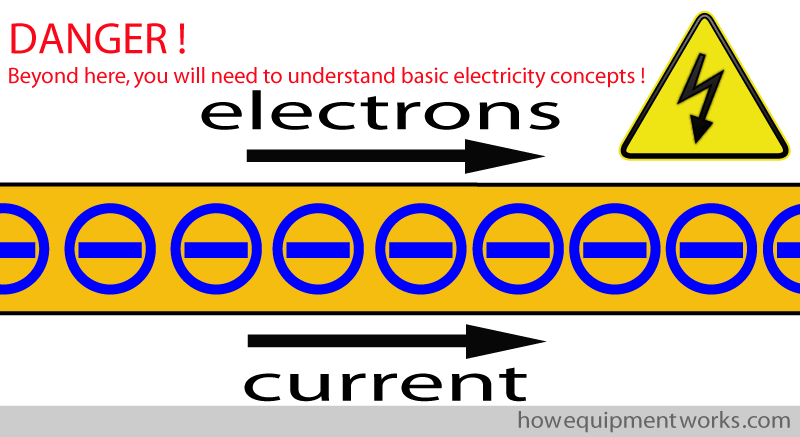
At this point, I would like to “warn” you that the discussion ahead will involve us dealing with some basic electrical concepts. Hopefully, this is not too surprising to you as defibrillation is all about electricity! However, do not worry too much if electricity frightens you as I will try and keep things as simple as possible. Also, this website has a separate section explaining the “basics of electricity”. If words like current, potential difference, alternating current and direct current make little sense to you, it might be a good idea to first visit the “basics of electricity” section of this website by clicking HERE (please remember to come back!).
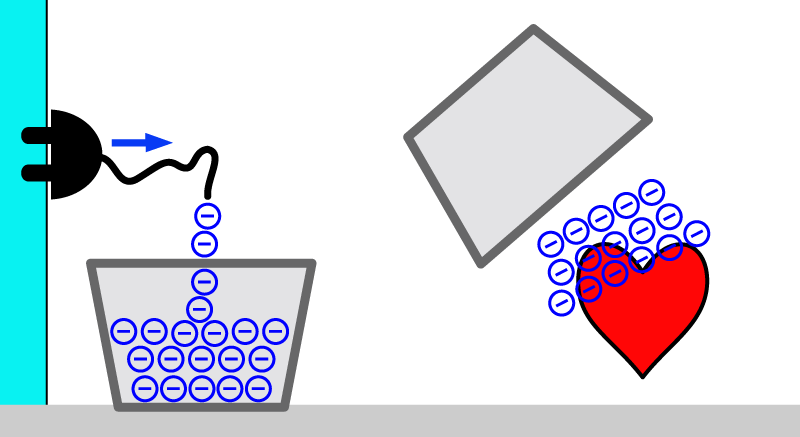
When you were a fireman, the bucket was the saviour. The defibrillator needs the electrical equivalent of the bucket. It needs something that can collect the continuous low flow of current from batteries or wall power and then release it as a brief large flow of current.
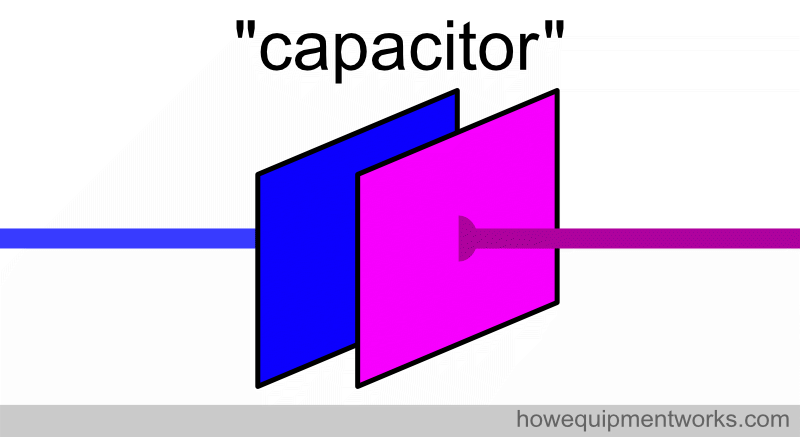
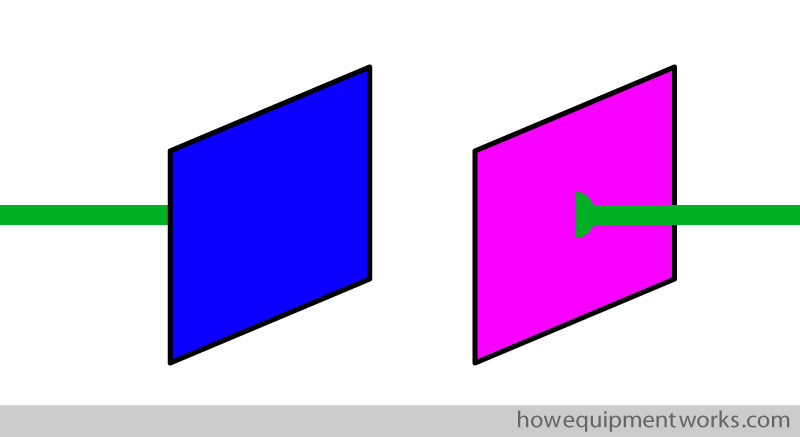
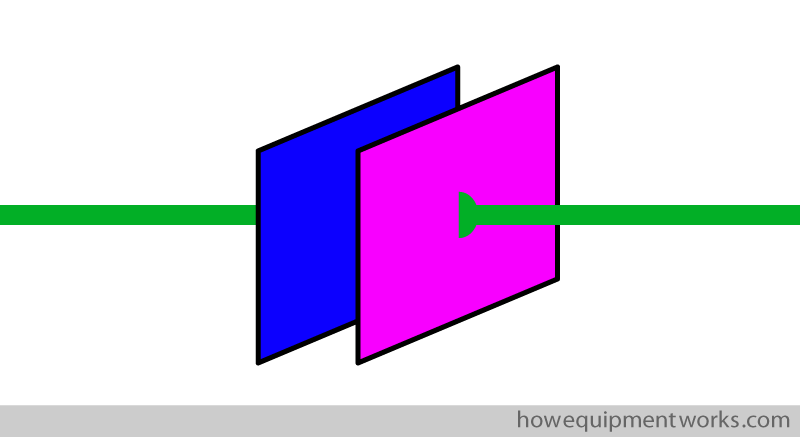
Fortunately, there is such a device and it is called a “capacitor”. Capacitors play an extremely important role in defibrillators and I will of course explain to you how they work. The capacitor in a defibrillator is able to collect the continuous low flow of current, store what it has collected, and then release it as the brief large flow of current needed for defibrillation. The basic design of a capacitor is extremely simple. It consists of two parallel flat metal plates, shown below as blue and pink squares. Wires (shown in green) are connected to each of the plates.

Do you work in the anaesthetic team? If you do, please visit the free website below, which has anaesthesia-related fun and safety material. Click the button below to visit.

The metal plates lie very closely next to each other. In real life, the plates are so close to each other that you would need a magnifying glass or microscope to see the separation. I, however, cannot draw them so close, so do remember to use your imagination when you see my diagrams.
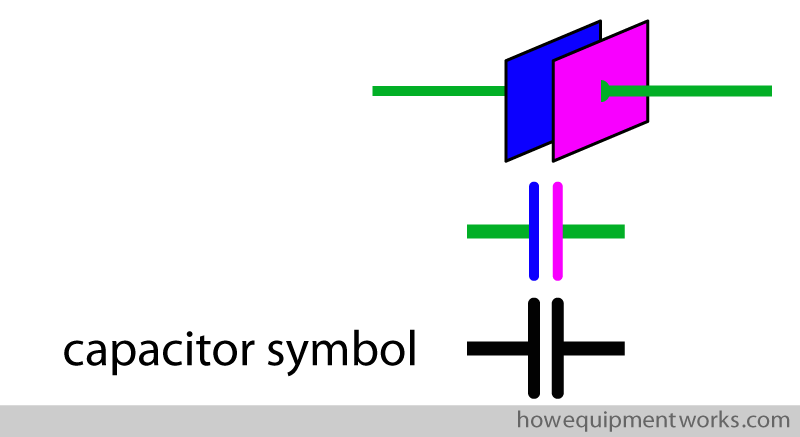
In the world of electronics, when a circuit is drawn, symbols are often used to represent various devices. Fortunately for us, the symbol representing a “capacitor” is very easy to remember as it looks so much like the object it represents.
How capacitors work
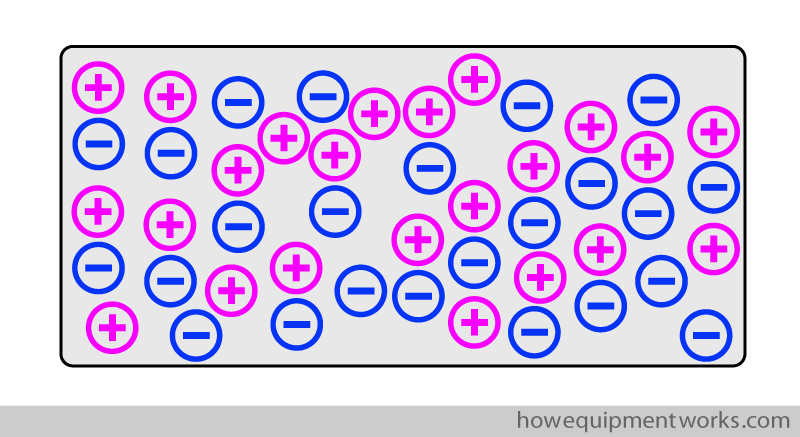
As explained before, a capacitor consists of two metal plates lying next to each other. To know how capacitors work, we need to first understand how a metal can become “electrically charged”. The actual physics of how this happens is somewhat complex and it is not necessary for our purposes to understand it in great detail. If you struggle to understand what I explain in this section, please just skip it and move on to the next section. Let us start! Metals have “positive charges” and “negative charges” inside them.
I would like you to, only for this discussion, think of the charges inside the metal as being very romantic boys and girls! The negative charges and positive charges are strongly attracted to each other. Given any opportunity, the opposite charges would love to form a relationship and be together as a happy couple!
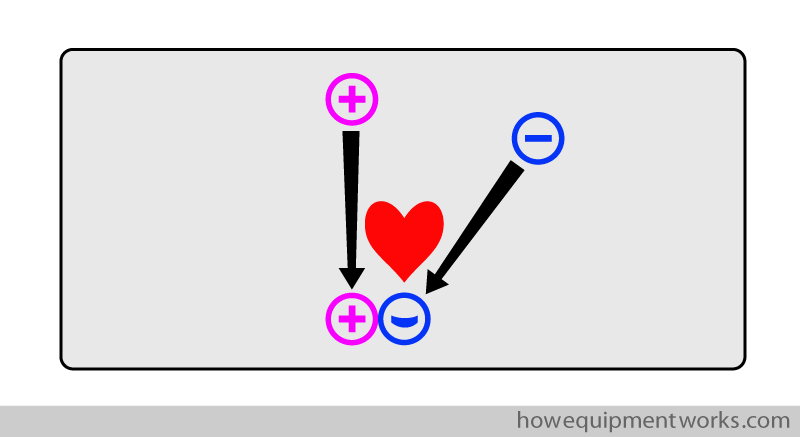
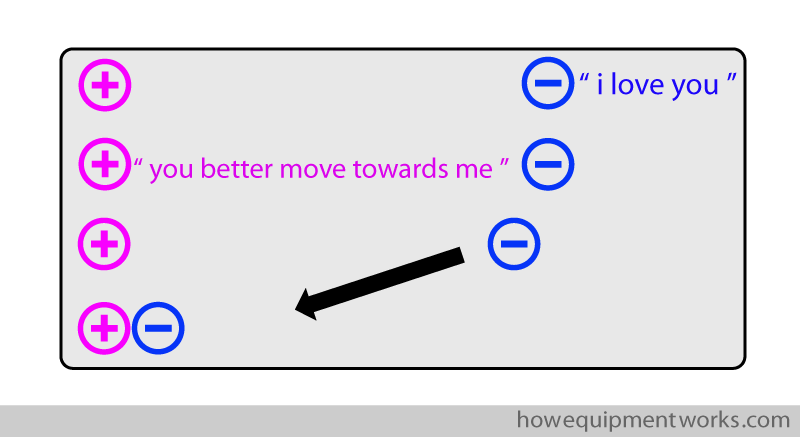
However, the positive charges are very “lazy”. Let me explain! Say that in the metal, there are positive charges at one end and there are negative charges at the other end. As explained before, the positive charges and negative charges are attracted to each other and they would like to be together to form a happy couple. In this situation, you would expect both charges to move towards each other.
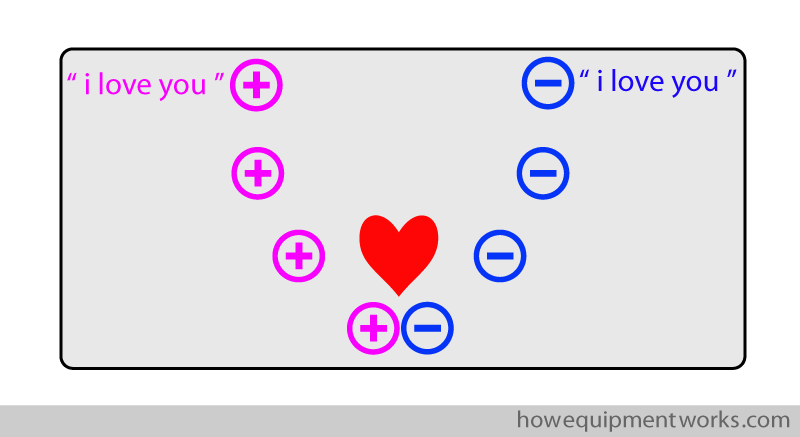
However, what happens is that only the negative charges move to be with the positive charges. The positive charges stay fixed in one place, which is why I call them “lazy”.
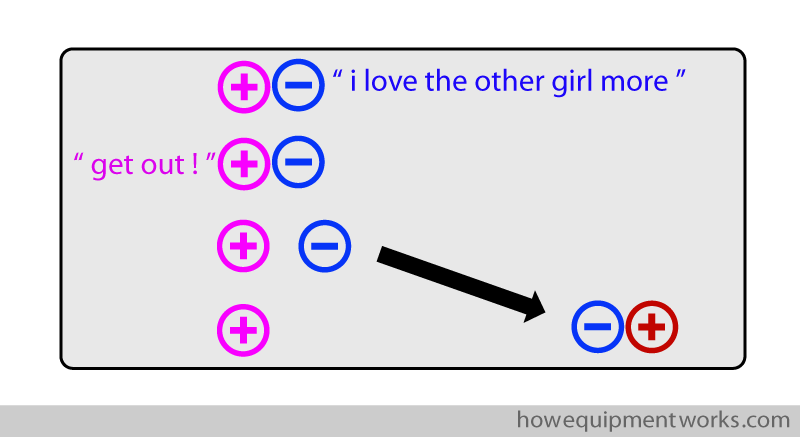
The same situation exists when a positive and negative charge couple split up. Say a negative charge is interested in another positive charge (negative charges are not very faithful !). When the negative charge leaves the positive charge to be with its new lover, the positive charge it was with will not “follow” it. It just lazily remains fixed in one place.
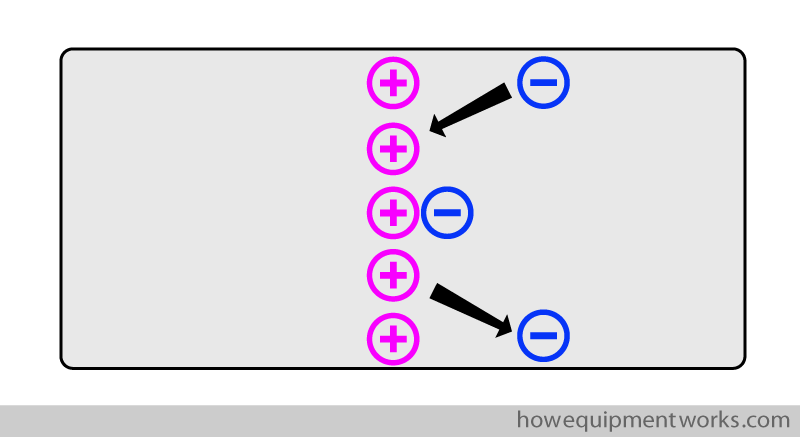
So basically, when attracted to each other or when leaving each other, it is only the negative charges that move.
From a physics point of view, we are not interested in the happy couples (i.e. where a negative charge is together with a positive charge). These “happy couples” (shown in grey below) are for the moment stable. What interests us are only the charges that do not have a partner (i.e. the ones who are lonely and are desperate for a partner, shown below with hearts). It is these single “available” charges that are active in electrical circuits.
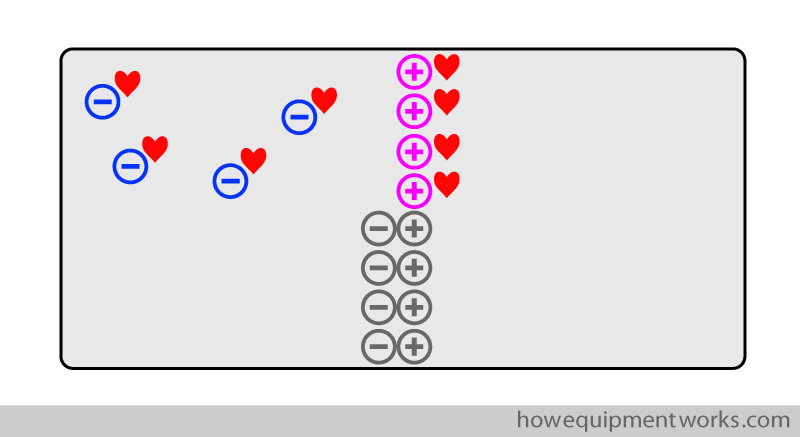
Now let us understand what we mean when we refer to the “charge” of a metal plate of a capacitor. Shown below is one metal plate of a capacitor. I have drawn this plate as a very thick one as this will help me to explain things better. A metal plate of a capacitor can have no charge, be positively charged, or be negatively charged. Let us first start by seeing a metal plate with “no charge”. Such a plate has an equal number of positive and negative charges inside it. Being “romantic”, these charges form “couples” and therefore there are no extra positive or negative charges left. As mentioned before, in physics, we are only interested in extra positive or negative charges. When we refer to the “charge ” of a metal plate, we are actually referring to how many extra “free” positive or negative charges are there. Since the metal capacitor plate in the example below has no extra charges, we can say that this plate has “no charge”.

Let us now make a capacitor by putting another metal plate next to the plate we saw before. Since this new metal plate also has no extra charges, we can also say that it has “no charge”.
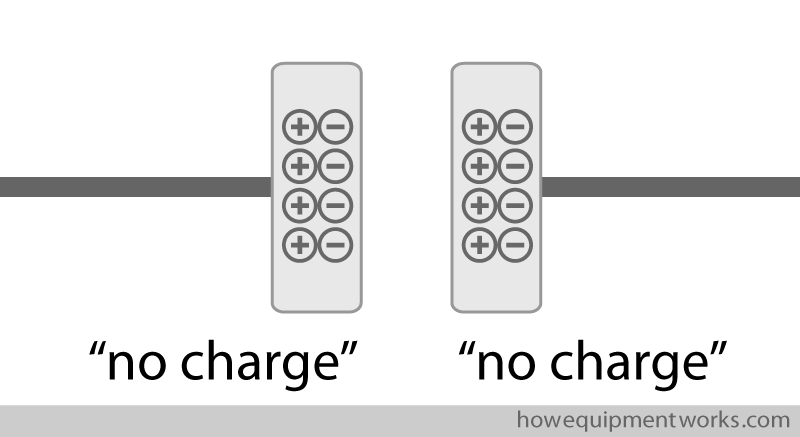
A capacitor with “no charge” in it has no energy for defibrillation. It is like an empty water bucket that needs to be filled before it can be used to put a fire out.
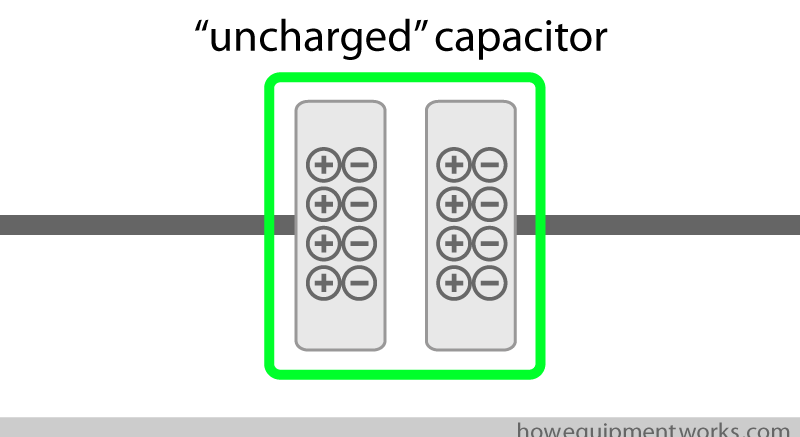
A capacitor needs to be “charged” before it can be used to provide current for defibrillation. Charging a capacitor is the equivalent of filling the bucket with water. During charging, electrons (i.e. current) goes into the capacitor and collect there (i.e. get stored).
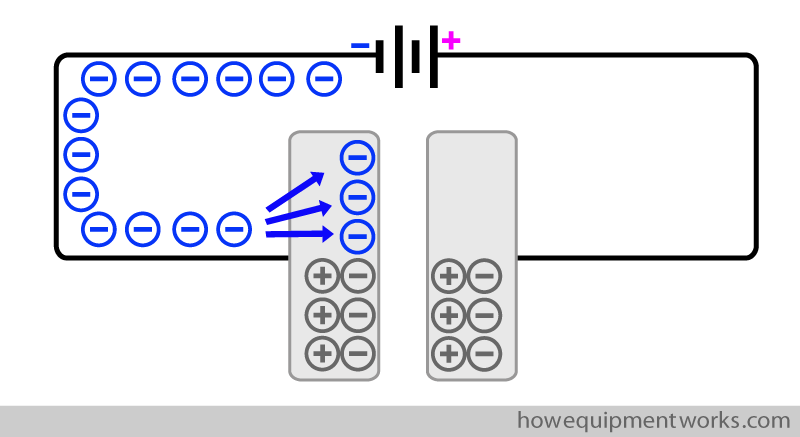
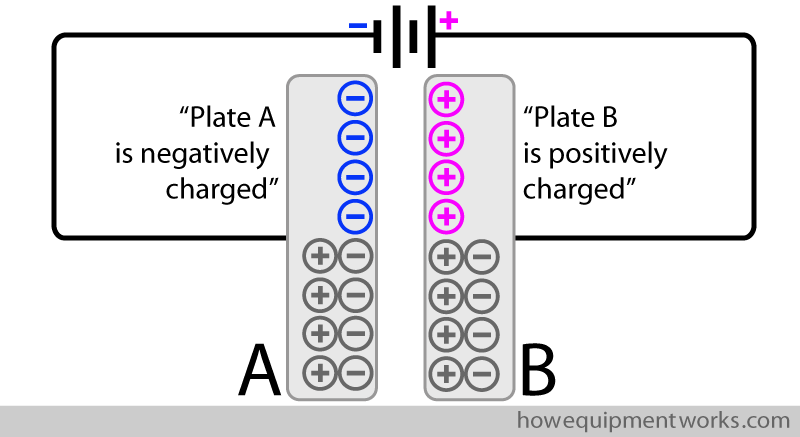
Shown below is a capacitor that has been “charged”. In this “charged” capacitor, plate A is “negatively charged” (because it has excess free negative charges) and plate B is “positively charged” (because it has excess free positive charges). In this charged state, the capacitor is capable of giving the necessary current required for defibrillation. In the sections that follow, I will explain to you how a capacitor is charged, and then, how it can release that charge (discharge).
Please click the “Next” button below to read part 2 about how defibrillators work. Thank you.