Note: This is part 2 of the discussion of how pulse oximeters work. If you have not read part 1, please click here to go to part 1.
Pulse oximeters measure pulsatile blood
In a body part such as a finger, arterial blood is not the only thing that absorbs light. Skin and other tissues also absorb some light. This poses a problem because the pulse oximeter should only analyse arterial blood while ignoring the absorbance of light by surrounding tissues. For an example of how tissues can interfere, take the two situations shown below. One is a thin finger and the other is a fat finger. The tissues in the thin finger absorb only a little extra light, while the fatter finger shown on the right absorbs much more light. However, the pulse oximeter has no way to measure whether the finger is fat or thin. It therefore has the potential to be confused because it doesn’t know how much light is absorbed by blood and how much is absorbed by the surrounding tissues.
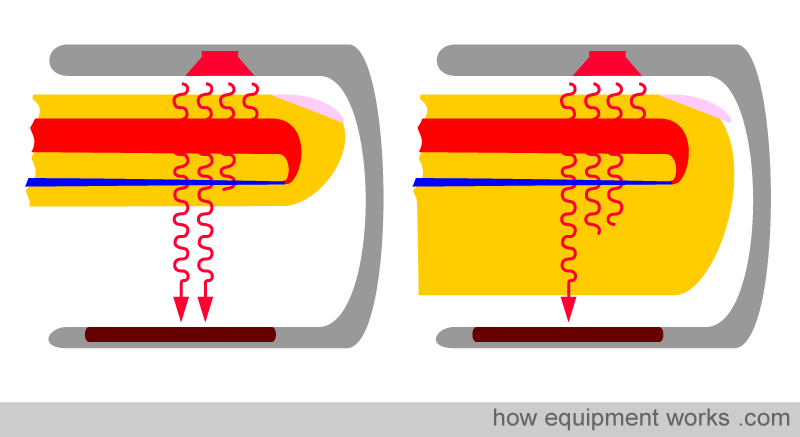
Fortunately, there is a clever solution to the problem. The pulse oximeter aims to analyse only arterial blood, disregarding the surrounding tissues. Luckily, arterial blood is the only thing pulsating in the finger. Everything else is non-pulsating. Any “changing absorbance” must therefore be due to arterial blood.
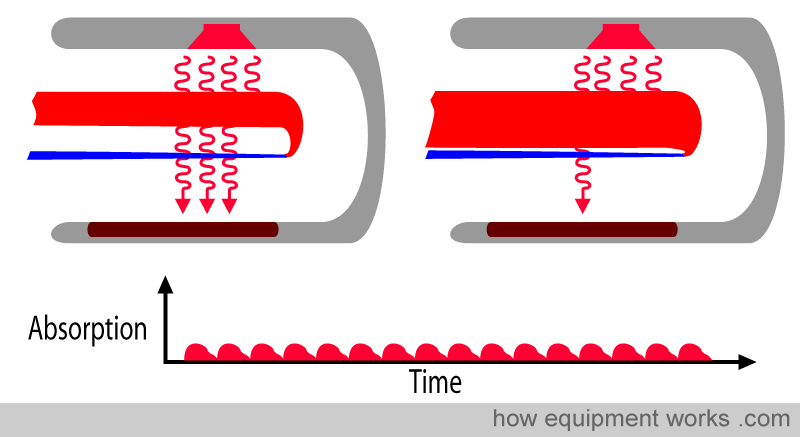
On the other hand, the pulse oximeter recognises that any absorbance that remains constant must be due to non-pulsatile factors, such as skin and other “non-arterial” tissues.
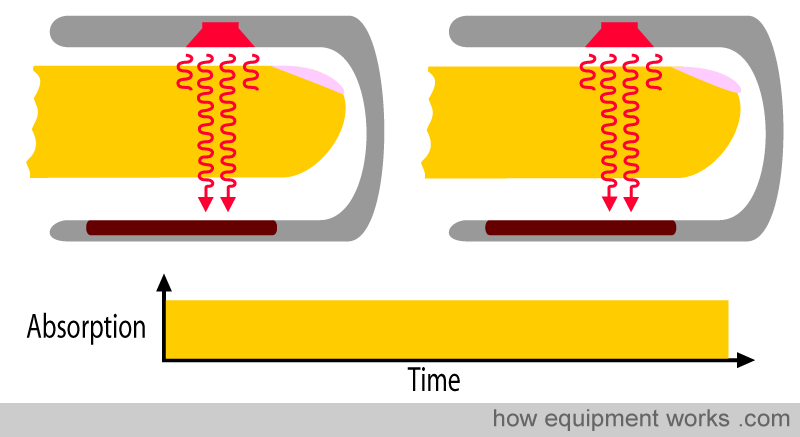
So the final signal picture reaching the pulse oximeter is a combination of the “changing absorbance” due to arterial blood and the “non-changing absorbance” due to other tissues.
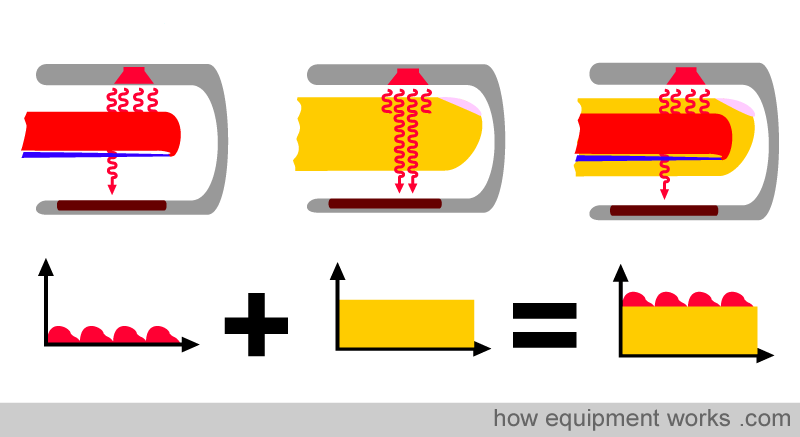
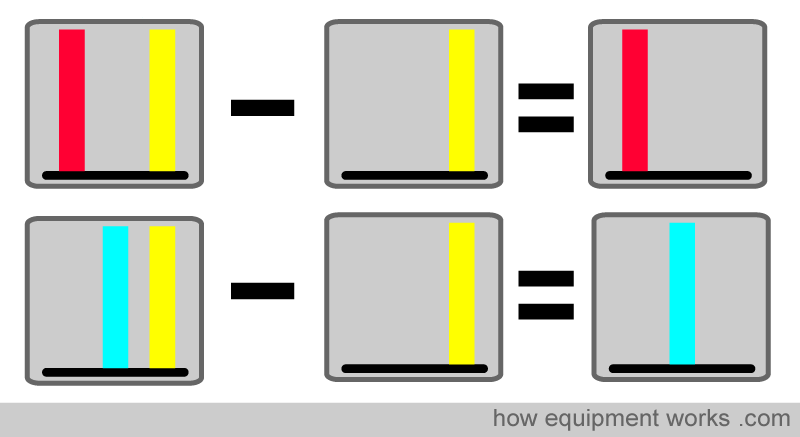
The pulse oximeter utilises clever mathematics to extract the “changing absorbance” signal from the total signal, as described below. As shown below, the computer subtracts the non-changing part of the absorbance signal from the total signal. After subtraction, only the “changing absorbance signal” remains, which corresponds to the pulsatile arterial blood. In this way, the pulse oximeter can calculate the oxygen saturation in arterial blood while ignoring the effects of surrounding tissues.
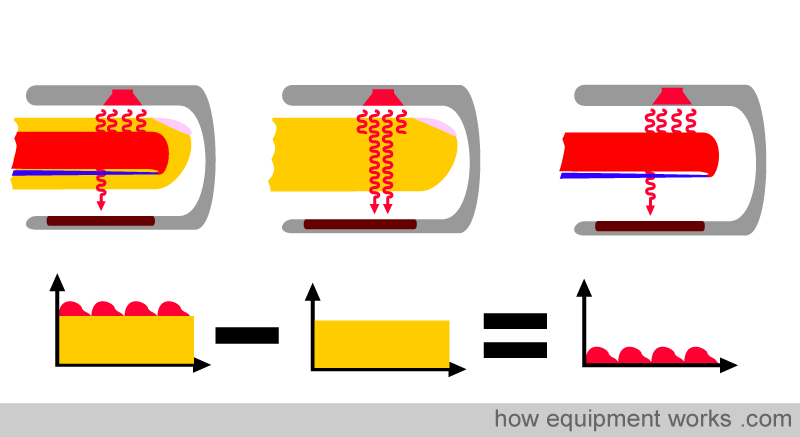
The signal is really small!
The diagrams used so far have exaggerated the size of the pulsatile part to make it easy for you to see and understand.
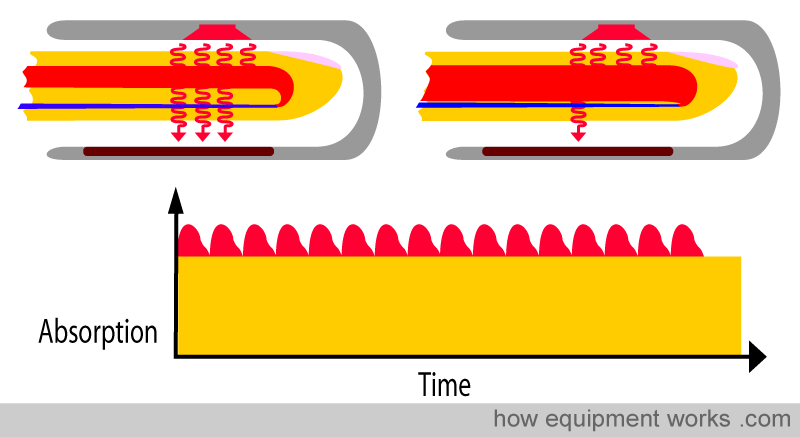
However, in reality, the pulsatile signal is very small. Typically, only about 2% of the total signal is pulsatile! Drawn to scale, 2% of the total signal will appear as shown in the diagram below. The orange part represents the “non-changing” light absorbed by the tissues. The red shows the changing absorbance due to pulsatile arterial blood. See how small this pulsatile signal is. Of all the light that passes through the finger, it is only the small pulsatile part that the pulse oximeter analyses. Because it represents such a small portion of the total light, the pulse oximeter is highly susceptible to errors if, for example, the probe is not placed properly or if the patient moves the probe.

Plethysmographic trace (Pleth)
Pulse oximeters often show the pulsatile change in absorbance in a graphical form. This is called the “plethysmographic trace ” or more conveniently, “pleth”.
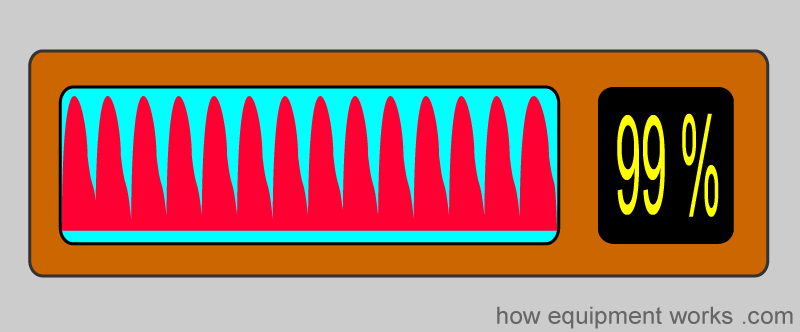
The pleth is an extremely important graph to see. It tells you how good the pulsatile signal is. If the quality of the pulsatile signal is poor, the calculation of oxygen saturation may be inaccurate. The pulse oximeter employs complex calculations to determine oxygen saturation. A poor pleth tracing can easily fool the computer into wrongly calculating the oxygen saturation. As human beings, we tend to believe what is good, so when we see a high saturation level, such as 99%, we are more likely to accept it, even if the patient’s actual saturation may be much lower. Always look at the pleth first, before checking oxygen saturation.
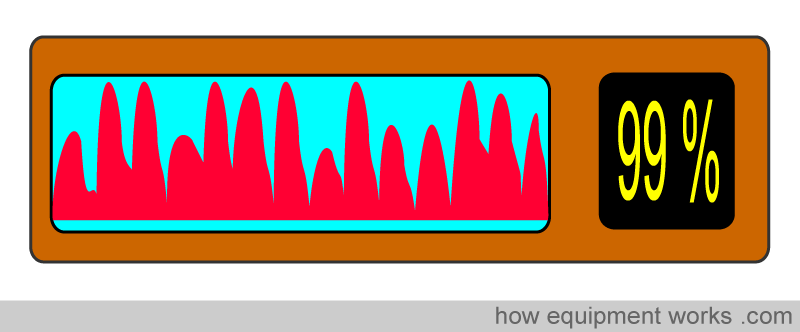
Never look only at oxygen saturation!

To remind you (okay, I promise, this is the last time!), think of “SpO2” as a reminder …..

The pleth is affected by factors that affect the peripheral blood flow. For example, low blood pressure or peripheral cold temperature can reduce it.
Sophisticated uses of the pleth are being developed. For example, it may be used to guide fluid therapy. These discussions are beyond the scope of this website.

Do you work in the anaesthetic team? If you do, please visit the free website below, which has anaesthesia-related fun and safety material. Click the button below to visit.

Light source
Pulse oximeters use a type of light source called “light emitting diodes” (LED), which are extremely commonly used in electronics.

Light-emitting diodes are ideal for pulse oximeters because :
- They are cheap ( so can be used even in disposable probes)
- They are very compact (can fit into very small probes)
- They emit light in accurate wavelengths
- They do not heat up much during use (low temperature makes it less likely to cause patient burns)
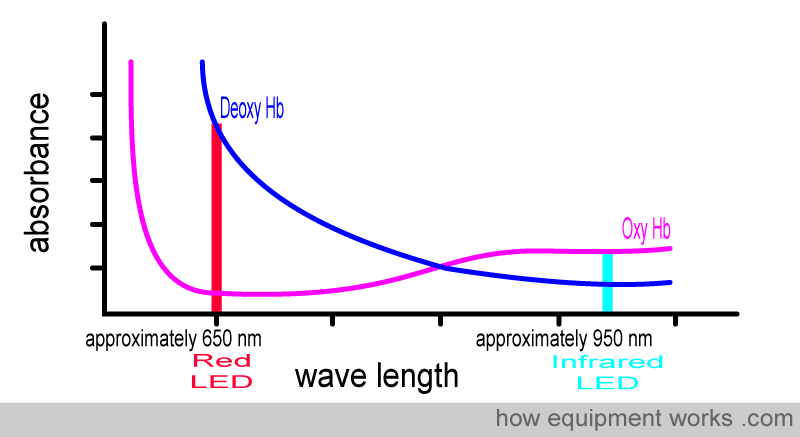
Light-emitting diodes come in a variety of types that emit light at specific wavelengths. Fortunately, there are light-emitting diodes (LEDs) that emit light in the red and infrared light wavelengths, and these are thus conveniently used in pulse oximeters. The exact wavelengths of the LEDs used depend on the manufacturer. For convenience, in our discussions, we assigned the red LED a wavelength of 650 nm and the infrared LED a wavelength of 950 nm (easy to remember). However, most textbooks will quote 660 nm and 940 nm.
Accounting for ambient (room) light
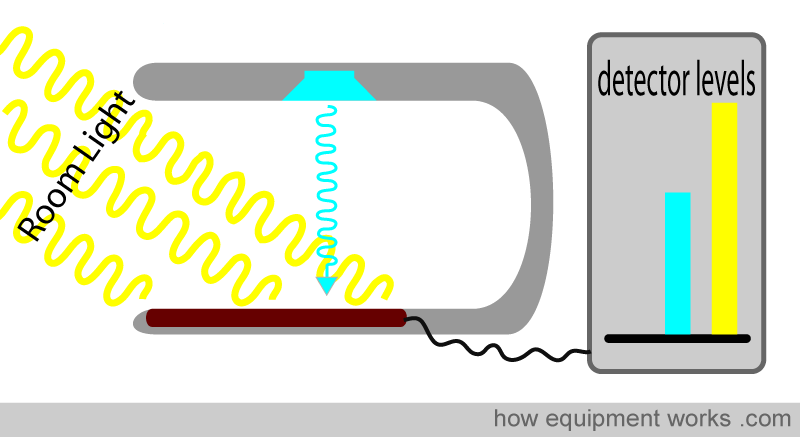
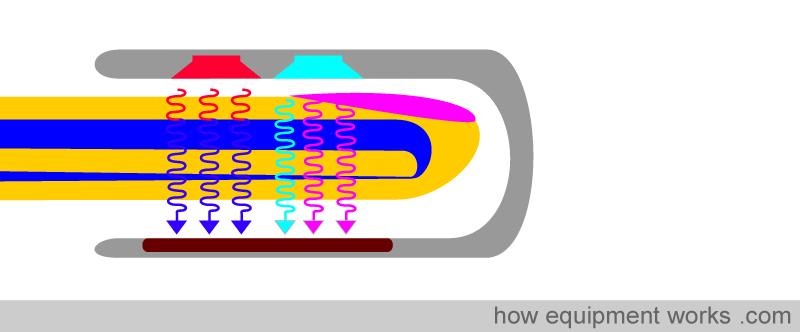
The pulse oximeter probe, as shown below, has a red LED and one infrared LED. On the other side is a light detector. However, you will note that, though there are only two LEDs, the light detector is exposed to three sources of light. In addition to the red and infrared LED light sources, there is also light in the room (ambient light) that the pulse oximeter is working in. Some of the light from this room can also reach the detector. The pulse oximeter has to work with these three sources of light. It wants the red and infrared light to calculate oxygen saturation. On the other hand, the room light is unwanted “noise” and needs to be taken into account. The process by which this is done will be explained.
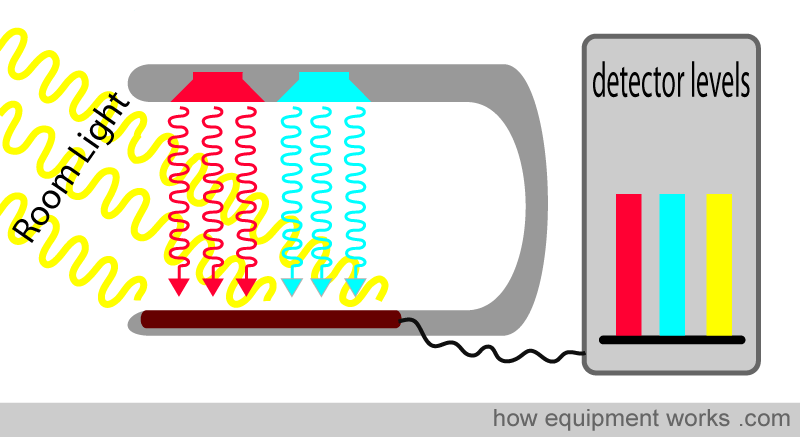
The above diagram illustrates both LEDs lit to facilitate the explanation. In reality, both LEDs are never lit together. Instead, the pulse oximeter rapidly switches the LEDs on and off in a particular sequence. First, the pulse oximeter activates the red LED light. The red light goes through the finger (not shown, to make the image less crowded) and reaches the detector. Stray room light also reaches the detector. The detector, therefore, records red light and room light that falls on it.
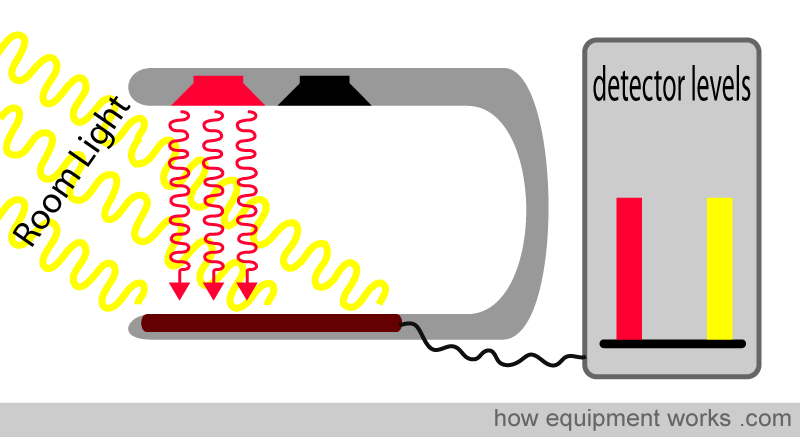
Next, the pulse oximeter switches off the red LED light and switches on the infrared LED light. The infrared light goes through the finger (not shown) and reaches the detector. Stray room light also reaches the detector. The detector therefore records infrared light and room light that falls on it.
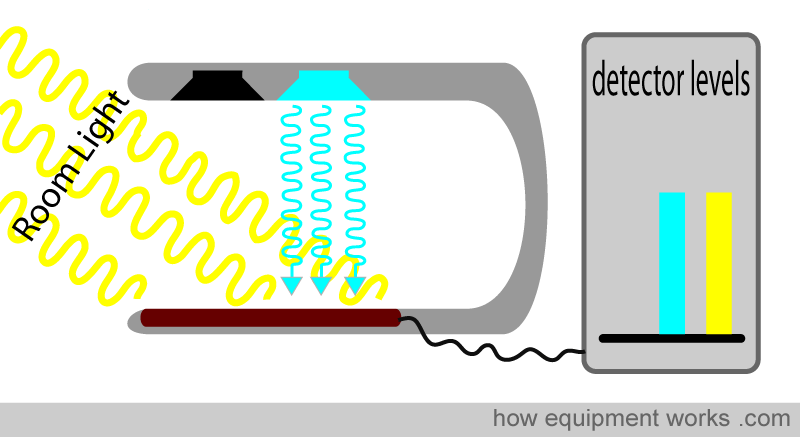
Finally, the pulse oximeter switches off both the red and infrared LED lights. Now, the only light that falls on the detector is the room light. The pulse oximeter now records the room light level.
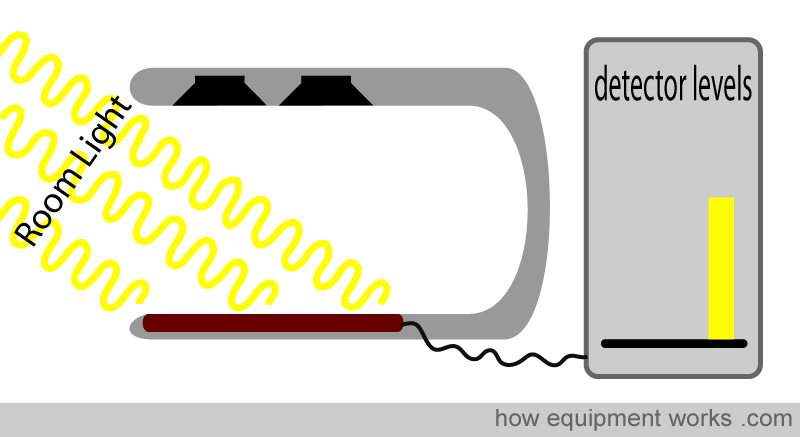
Because the pulse oximeter now knows the level of room light, it can subtract it from the readings to get the actual red and infrared light levels.
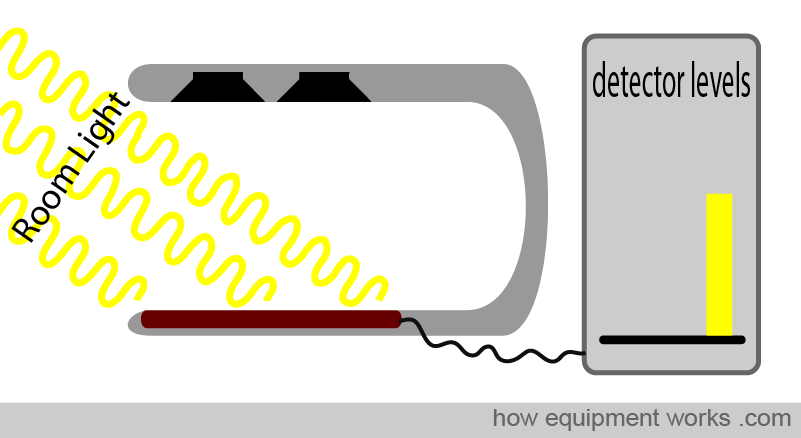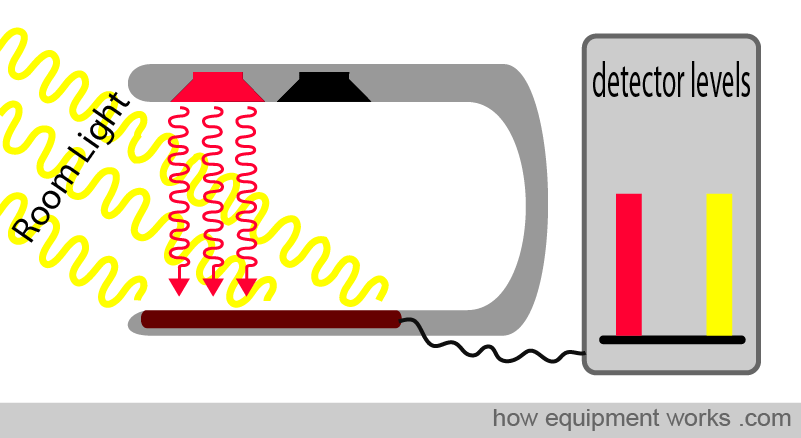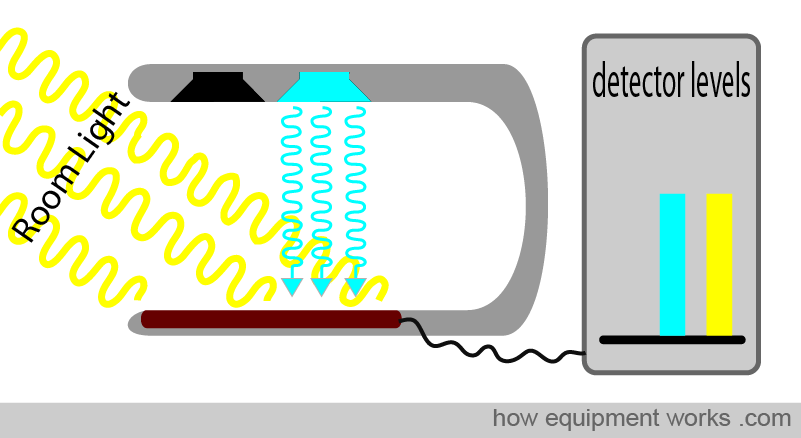
The animation below shows the LEDs switching on and off in sequence. The animation is shown in slow motion to make it easy to understand. In reality, this switching happens hundreds of times per second.
So here is the sequence:
Only the red LED is on. The sensor measures the red light plus the room light.
Only the infrared LED is on. The sensor measures the infrared light plus the room light.
Both LEDs are off. The sensor measures only the room light.
Problems with the pulse oximeter
Problem of movement
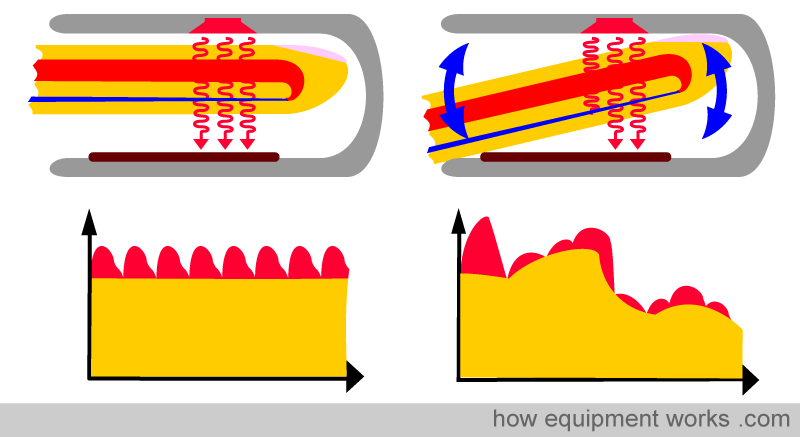
When considering problems associated with pulse oximeters, it is essential to remember that the signal being analysed is tiny. As explained before, it is only about 2 % of the total light that is analysed.

With such a small signal, it is easy to see how errors can occur. Pulse oximeters are highly susceptible to motion, such as a patient moving their hand. As the finger moves, the light levels change dramatically. Such a poor signal makes it difficult for the pulse oximeter to calculate oxygen saturation.
The problem of optical shunting
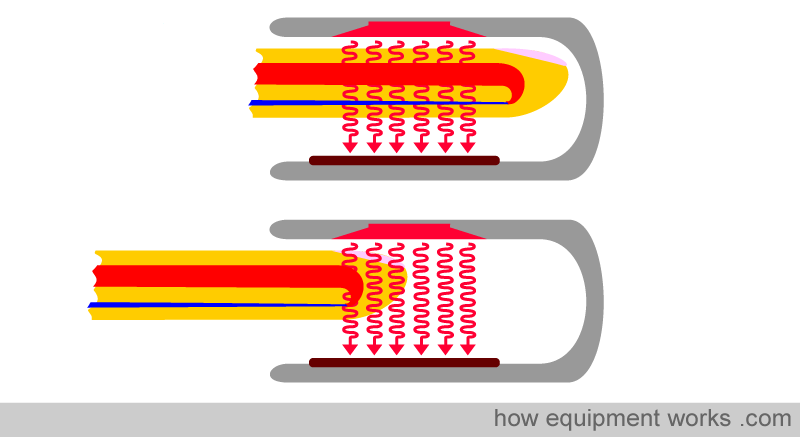
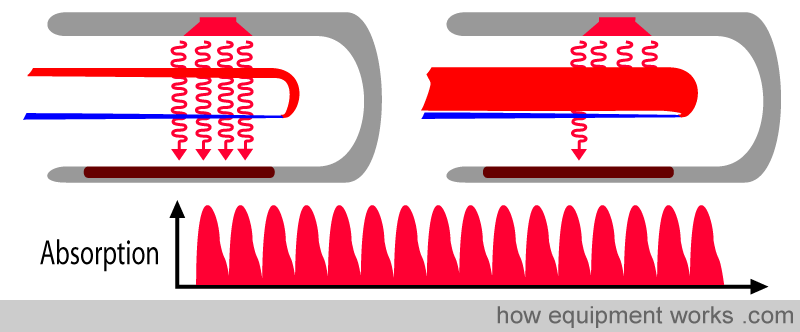
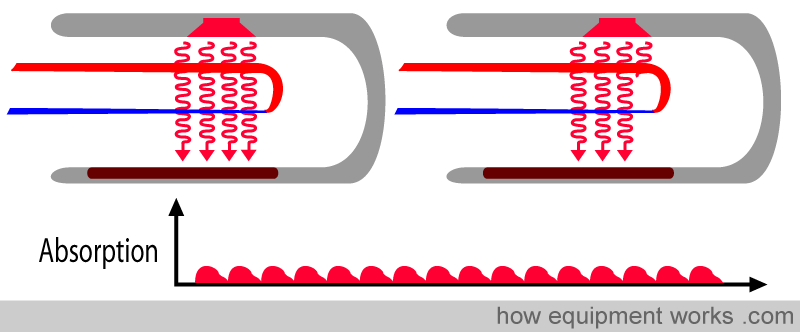
The pulse oximeter operates most effectively when all the light passes through arterial blood, as illustrated by the upper finger in the image below. However, if the probe is of the wrong size or has not been appropriately applied, some of the light, instead of going through the artery, goes by the side of the artery (shunting)(lower finger in the image below). This reduces the strength of the pulsatile signal, making the pulse oximeter prone to errors. It is therefore essential to select the correctly sized probe and to position the finger correctly within the chosen probe for optimal results.
The problem of too much ambient light
As discussed before, in addition to the light from the LEDs, ambient (room) light also hits the detector. For the pulse oximeter to function correctly, the strength of the LED light falling on the detector should be good when compared to the strength of the ambient light falling on the detector.
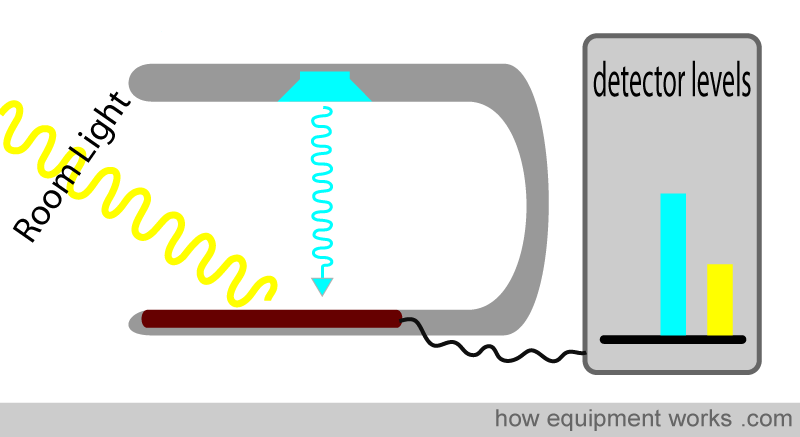
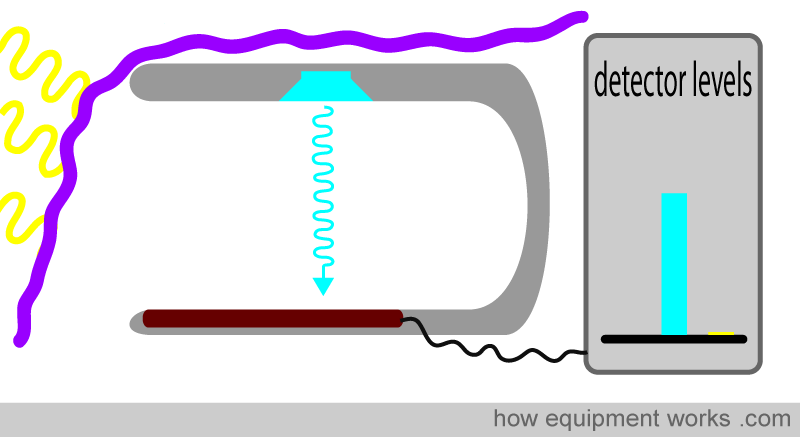
If the ambient light is too strong, the LED light signal gets “submerged” in the noise of the ambient light. This can lead to erroneous readings.
Therefore, it is important to minimise the amount of ambient light falling on the detector. One can try to move the probe away from strong sources of room light. One can also try to cover the pulse oximeter probe and finger with a cloth, etc.
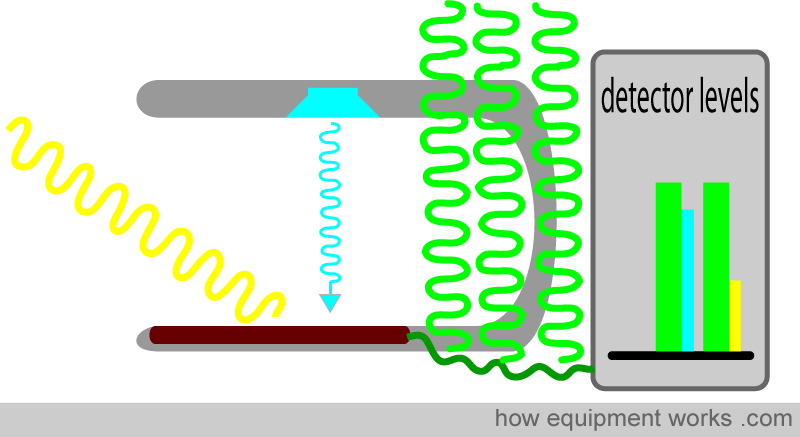
The problem of electromagnetic interference
Electrical equipment such as surgical diathermy emits strong electric waves, which the wires of the pulse oximeter may pick up. These waves (shown in green below) cause small currents to form in the wires, confusing the pulse oximeter, which assumes these currents originate from the light detector. When using diathermy, one should exercise caution when interpreting pulse oximeter readings.
The problem of poor peripheral perfusion
Good peripheral blood flow makes the arteries in the fingers appear nicely pulsatile. As previously discussed, it is the pulsatile change in absorbance that is used in calculating oxygen saturation.
When peripheral perfusion is poor (e.g., in hypotension), the arteries are significantly less pulsatile. The change in absorbance is therefore less, and the pulse oximeter may then find the signal inadequate to correctly calculate oxygen saturation.
The problem of not detecting hyperoxia
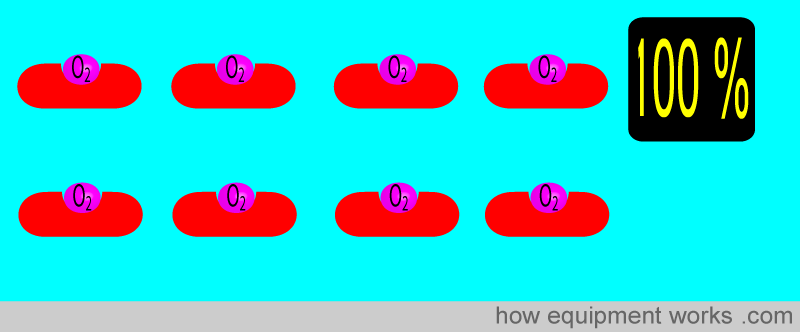
Initially, we discussed that oxygen saturation refers to the percentage of haemoglobin that is carrying oxygen. In the example below, all the haemoglobin is carrying oxygen, and therefore the oxygen saturation is 100 %.
However, haemoglobin is not the only way oxygen is carried in the blood. Additional oxygen can also be dissolved in the solution in which red blood cells travel (plasma). The problem is that the pulse oximeter cannot “see” the extra dissolved oxygen. So, even though this patient’s blood is full of extra oxygen, the saturation still shows 100%, instead of, say, 120%.
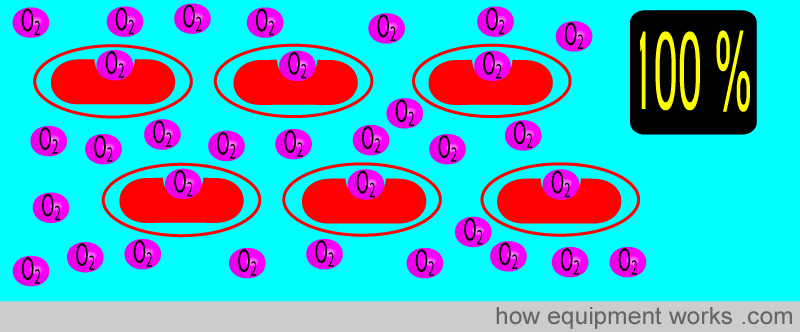
The 100 % saturation in the above example tells us that the patient is getting enough oxygen. However, it does not indicate that the patient is receiving too much oxygen (hyperoxia). Oxygen, while necessary for life, can be harmful if given in excess. Therefore, other means (e.g. arterial blood gas) have to be used to detect hyperoxia.
Problem of calibration
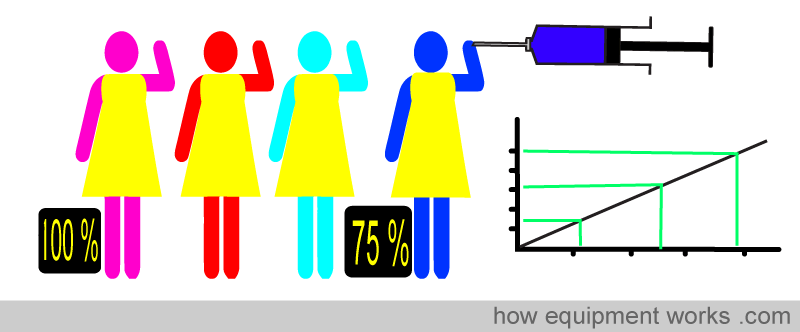
As mentioned earlier, pulse oximeters are calibrated using human subjects. This means that low saturations may not be accurate.
Problem of Colored dyes and nail polish
The dye, methylene blue, if in the patient’s circulation, will artificially lower the displayed oxygen saturation. Fingernail polish can affect the accuracy of saturation determination.
Problem of abnormal haemoglobins
Abnormal haemoglobin can affect pulse oximeter readings. Carbon monoxide combines with haemoglobin to form carboxyhaemoglobin. Most pulse oximeters cannot separately detect carboxyhaemoglobin. Instead, it considers carboxyhemoglobin as oxyhemoglobin. This is dangerous because carboxyhemoglobin doesn’t carry oxygen, and the artificially high oxygen saturation displayed may wrongly reassure everyone. Another abnormal haemoglobin, called methemoglobin, causes the saturation to falsely show readings towards about 85 %
We have now reached the end of our discussion on pulse oximetry. I hope it has provided you with a good introduction to the subject and will be helpful as you read further on this topic. This website is primarily funded by donations, so if you can help, please consider making a small contribution as described below. Additionally, I don’t have an advertising budget, so please share this website with your colleagues, near and far. Thank you very much.

Hello! My name is Pras, and I am the author of this website. I have made the website completely free to access so that people from all over the world can benefit from it.
If you can afford it, I would be very grateful if you would consider making a single donation of one dollar (or the equivalent in your currency) to help cover the expenses needed to run this website (e.g. for special software and computers). For this website to survive, donations are desperately needed. Sadly, without donations, this website may have to be closed down.
Unfortunately, perhaps because many people think that someone else will donate, this website gets only very few donations. If you are able to, please consider making a single donation equivalent to one dollar. With support from people like you, I am sure this educational website will continue to survive and grow. Thank you very much for your support.

